Inspired Skin+Wellness | Dermatology
Kathileen Boozer, DNP, APRN, FNP-C
Nurse Practitioner
Common Skin Conditions List
Educational & Information Purposes

Hair Loss
Hair Loss: Overview
Hair loss, also known as alopecia, refers to the partial or complete loss of hair from the scalp or other parts of the body. It can affect both men and women and may occur gradually or suddenly.
Common Causes of Hair Loss
Genetic Factors: Hereditary conditions such as male-pattern baldness and female-pattern baldness.
Hormonal Changes: Conditions like pregnancy, childbirth, menopause, and thyroid issues.
Medical Conditions: Autoimmune diseases, scalp infections, and other health issues.
Medications: Certain drugs for cancer, arthritis, depression, heart problems, and high blood pressure.
Physical or Emotional Stress: Significant stress can trigger temporary hair loss.
Nutritional Deficiencies: Lack of essential nutrients like iron, protein, and vitamins.
Hairstyling Practices: Excessive styling, heat, and chemical treatments can damage hair.
Possible Work-Up for Hair Loss
Medical History: Review of the patient’s personal and family history of hair loss.
Physical Examination: Inspection of the scalp and hair to assess the pattern and extent of hair loss.
Blood Tests: To check for underlying conditions such as thyroid issues or nutritional deficiencies.
Scalp Biopsy: In some cases, a small sample of scalp skin may be taken for analysis.
Pull Test: To determine the extent of hair loss by gently pulling on a few strands.
Treatment Options for Hair Loss
Medications:Minoxidil (Rogaine): A topical solution applied to the scalp.
Finasteride (Propecia): An oral medication for men that inhibits hair lossLaser Therapy: Low-level laser therapy may stimulate hair growth.
Platelet-Rich Plasma (PRP) Therapy: Involves injecting a concentration of platelets to promote hair growth.
Hair Transplant Surgery: A procedure that moves hair follicles from one part of the body to the balding area.
Recommendations
Consult a Healthcare Professional: For personalized advice and to rule out underlying health issues.
Maintain a Healthy Diet: Ensure adequate intake of vitamins and minerals essential for hair health.
Avoid Harsh Hair Treatments: Limit the use of heat styling tools and chemical treatments.
Manage Stress: Engage in stress-reducing activities like exercise, meditation, or hobbies.
Be Gentle with Hair: Use a soft brush and avoid tight hairstyles that can cause traction alopecia.

Contact Dermatitis
What is Contact Dermatitis?
Contact dermatitis is a type of inflammation of the skin that occurs when the skin comes into contact with a substance that causes an allergic reaction or irritation. It can be classified into two main types: allergic contact dermatitis and irritant contact dermatitis.
What Does Contact Dermatitis Look Like?
The appearance of contact dermatitis can vary depending on the cause and the individual's skin type. Common symptoms include:
Redness
Itching
Swelling
Blisters
Dry, scaly patches
Crusting or oozing in severe cases
Possible Treatments
Treatment for contact dermatitis typically involves:
Avoiding the irritant or allergen
Topical corticosteroids to reduce inflammation
Oral antihistamines to relieve itching
Moisturizers to soothe the skin
In severe cases, systemic corticosteroids may be prescribed
Recommendations
To manage and prevent contact dermatitis, consider the following recommendations:
Identify and avoid known triggers.
Use protective clothing or gloves when handling irritants.
Maintain skin hydration with regular use of moisturizers.
Perform patch testing with a dermatologist if allergic contact dermatitis is suspected.
Consult a healthcare provider for persistent or severe cases.
Picture Source: https://dermnetnz.org/topics/contact-dermatitis

Cysts
Pilar Cyst: Overview
A pilar cyst, also known as a trichilemmal cyst, is a type of benign cyst that typically forms on the scalp. These cysts arise from hair follicles and are filled with keratin, a protein that is a key component of hair and skin.
Appearance
Pilar cysts generally have the following characteristics:
Round or dome-shaped lumps
Skin-colored or slightly yellowish
Firm to the touch
Usually painless, though they can become tender if infected
Commonly found on the scalp but can appear elsewhere on the body
Treatment Options
While pilar cysts are usually harmless and do not require treatment, options include:
Observation: If the cyst is not causing discomfort, it may simply be monitored.
Incision and drainage: If the cyst becomes painful or infected, a healthcare provider may drain it.
Surgical removal: For persistent or bothersome cysts, complete surgical excision may be recommended to prevent recurrence.
Recommendations
If you suspect you have a pilar cyst or experience any discomfort, consider the following recommendations:
Consult a dermatologist for an accurate diagnosis.
Avoid squeezing or trying to pop the cyst, as this can lead to infection.
Keep the area clean and monitor for any changes.
Discuss treatment options with a healthcare provider if the cyst becomes bothersome.
picture source: https://dermnetnz.org/topics/trichilemmal-cyst

Fungal Infection
Fungal Infection: Overview
A fungal infection is caused by the overgrowth of fungi, which are microorganisms that can thrive in various environments. These infections can affect different parts of the body, leading to a range of symptoms and health issues.
Common Areas Affected by Fungal Infections
Skin: Commonly seen as athlete's foot, ringworm, and candidiasis.
Nails: Fungal nail infections can cause discoloration, thickening, and separation from the nail bed.
Genital Area: Yeast infections are common in both men and women.
Oral Cavity: Oral thrush, caused by Candida, presents as white patches in the mouth.
Appearance of Fungal Infections
Skin: Red, itchy patches, scaling, or blisters.
Nails: Discoloration (yellow, brown), brittleness, or crumbling.
Genital Symptoms: Itching, burning, and unusual discharge.
Oral Thrush: White, creamy lesions on the tongue and inner cheeks.
Possible Treatments for Fungal Infections
Topical Antifungals: Creams or ointments applied directly to the affected area.
Oral Antifungals: Pills prescribed for more severe or widespread infections.
Medicated Shampoos: Used for scalp fungal infections.
Home Remedies: Some may find relief using natural antifungal agents like tea tree oil or garlic.
Recommendations to Prevent Fungal Infections
Maintain Hygiene: Keep skin clean and dry, especially in warm, moist areas.
Avoid Sharing Personal Items: Do not share towels, shoes, or personal grooming items.
Wear Breathable Fabrics: Choose clothing made of cotton or moisture-wicking materials.
Manage Underlying Health Conditions: Control diabetes and other conditions that may increase susceptibility.
Consult a Healthcare Provider: Seek medical advice if symptoms persist or worsen.
Picture Source: https://dermnetnz.org/topics/candidiasis-of-skin-folds

Hives
What are Hives?
Hives, also known as urticaria, are raised, itchy welts on the skin that can vary in size and shape. They can appear anywhere on the body and are often red or skin-colored. Hives can be acute, lasting less than six weeks, or chronic, persisting for six weeks or longer.
What Do Hives Look Like?
Hives typically present as:
Raised, swollen areas on the skin
Red or pale in color
Itchy and sometimes painful
Can vary in size from small spots to large patches
Common Causes of Hives
Hives can be triggered by a variety of factors, including:
Allergic reactions to foods (e.g., nuts, shellfish)
Insect stings or bites
Medications (e.g., antibiotics, non-steroidal anti-inflammatory drugs)
Infections (e.g., viral infections)
Environmental factors (e.g., pollen, pet dander)
Physical triggers (e.g., pressure, temperature changes)
Treatments for Hives
Treatment options for hives may include:
Antihistamines to relieve itching and swelling
Topical corticosteroids for localized inflammation
Oral corticosteroids for severe cases
Omalizumab (Xolair) for chronic hives not responding to other treatments
Recommendations
To manage and prevent hives, consider the following recommendations:
Avoid known triggers and allergens
Wear loose-fitting clothing to reduce irritation
Keep the skin moisturized to reduce itchiness
Use cool compresses to soothe the skin
Consult a healthcare professional for persistent or severe cases
Picture Source: https://dermnetnz.org/topics/urticaria-an-overview
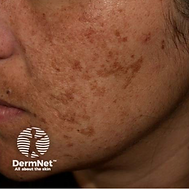
Melasma
What is Melasma?
Melasma is a common skin condition characterized by the appearance of brown or gray-brown patches on the skin, primarily on the face. It occurs when the skin produces excess melanin, the pigment responsible for skin color. Melasma is often triggered by factors such as sun exposure, hormonal changes (especially during pregnancy or with contraceptive use), and certain medications.
What Does Melasma Look Like?
Melasma typically appears as symmetrical patches on the face, commonly affecting the:
Cheeks
Forehead
Nose
Chin
The patches can vary in size and may be more pronounced in individuals with darker skin tones. The condition is not harmful but can be a source of cosmetic concern for many.
Possible Treatments for Melasma
Treating melasma often requires a combination of approaches. Here are some common treatments:
Topical Treatments: Creams containing hydroquinone, tretinoin, or corticosteroids can help lighten the patches.
Chemical Peels: These treatments use acids to exfoliate the skin and can improve the appearance of melasma.
Laser Therapy: Certain laser treatments can target melanin and reduce pigmentation.
Microneedling: This procedure can stimulate collagen production and improve skin texture and tone.
Skincare Regimen for Melasma
A consistent skincare regimen can help manage melasma. Here are the recommended steps:
Gentle Cleanser: Use a mild, non-irritating cleanser to avoid aggravating the skin.
Exfoliation: Incorporate gentle exfoliants 1-2 times a week to promote cell turnover.
Brightening Serums: Look for serums containing vitamin C or niacinamide to help brighten the skin.
Moisturizer: Keep the skin hydrated with a non-comedogenic moisturizer.
Sun Protection: Apply a broad-spectrum sunscreen with SPF 30 or higher daily to protect against UV rays, which can worsen melasma.
Medical Grade Product Recommendations: ZO Skin Health
ZO Skin Health offers several medical-grade products that may be beneficial for treating melasma:
ZO Skin Health Brightalive: A skin tone evening cream that helps reduce the appearance of discoloration.
ZO Skin Health Daily Skin Care Program: A comprehensive regimen that includes cleansing, exfoliation, and protection.
ZO Skin Health Pigment Control Crème: A targeted treatment designed to reduce the appearance of dark spots and improve skin tone.
ZO Skin Health Sunscreen: A broad-spectrum sunscreen that provides essential protection against UV damage.
Always consult with a dermatologist before starting any new treatment or skincare regimen to ensure it is appropriate for your skin type and condition.

Nail Disease
Nail Disease: Overview
Nail diseases encompass a variety of conditions that affect the appearance, structure, and health of the nails. These conditions can be caused by infections, underlying health issues, or environmental factors.
What Nail Diseases Look Like
Nail diseases can manifest in several ways, including:
Discoloration: Nails may turn yellow, green, or brown.
Thickening: Nails can become thicker than normal.
Cracking or Splitting: Nails may crack or split easily.
Separation: The nail may separate from the nail bed (onycholysis).
Pitting: Small dents or pits may appear on the surface of the nails.
Ridges: Vertical or horizontal ridges may develop.
Possible Treatments
Treatment for nail diseases depends on the underlying cause. Some common treatments include:
Antifungal Medications: Used for fungal infections.
Topical Treatments: Creams or ointments for localized conditions.
Oral Medications: Prescribed for severe infections or systemic issues.
Laser Therapy: Used for certain fungal infections.
Moisturizers: To prevent dryness and cracking.
Dietary Changes: Ensuring proper nutrition to support nail health.
Recommendations for Nail Health
To maintain healthy nails and prevent nail diseases, consider the following recommendations:
Keep Nails Clean and Dry: Regularly wash and dry your hands and nails.
Moisturize: Use hand creams or oils to keep nails and cuticles hydrated.
Avoid Harsh Chemicals: Limit exposure to detergents and cleaning products.
Wear Protective Gloves: When using chemicals or doing household chores.
Maintain a Balanced Diet: Include vitamins and minerals that promote nail health, such as biotin, zinc, and protein.
Consult a Healthcare Professional: If you notice persistent changes in your nails, seek medical advice.

Pre-Cancers (Actinic Keratosis)
What is Actinic Keratosis?
Actinic keratosis (AK) is a rough, scaly patch on the skin that develops due to prolonged exposure to ultraviolet (UV) light, primarily from the sun. It is considered a precancerous condition, as it can potentially progress to squamous cell carcinoma if left untreated.
What Does Actinic Keratosis Look Like?
Actinic keratosis typically appears as:
Small, rough, red, or brown patches on sun-exposed areas of the skin, such as the face, ears, neck, scalp, and backs of the hands.
Dry, scaly, or crusty texture.
Size can vary from a few millimeters to a centimeter or more.
It may be itchy or tender, but often it is asymptomatic.
How Do You Get Actinic Keratosis?
Actinic keratosis develops primarily due to:
Chronic sun exposure, especially without adequate protection.
Use of tanning beds.
Living in sunny climates or high altitudes.
Having fair skin, light hair, and light eyes, which are more susceptible to sun damage.
A weakened immune system, which can increase the risk of skin damage.
Risks Associated with Actinic Keratosis
Individuals at higher risk for developing actinic keratosis include:
People over the age of 40.
Individuals with a history of sunburns or excessive sun exposure.
Those with a family history of skin cancer.
People with certain medical conditions that weaken the immune system.
Treatments for Actinic Keratosis
Treatment options for actinic keratosis may include:
Topical medications such as 5-fluorouracil (5-FU) or imiquimod.
Cryotherapy, which involves freezing the lesion with liquid nitrogen.
Photodynamic therapy, which uses light to activate a photosensitizing agent applied to the skin.
Laser therapy to remove the affected skin layers.
Excisional surgery to remove larger lesions.
Self-Care for Actinic Keratosis
To manage and prevent actinic keratosis, consider the following self-care tips:
Apply broad-spectrum sunscreen with an SPF of 30 or higher daily, even on cloudy days.
Avoid direct sunlight during peak hours (10 a.m. to 4 p.m.).
Wear protective clothing, hats, and sunglasses when outdoors.
Regularly check your skin for new or changing lesions and consult a healthcare provider if you notice any concerning changes.
Consider regular dermatological check-ups, especially if you have a history of skin damage or AK.
Picture Source: https://dermnetnz.org/topics/actinic-keratosis

Skin Cancers
Understanding Skin Cancers
Skin cancer is one of the most common types of cancer, primarily caused by exposure to ultraviolet (UV) radiation from the sun or tanning beds. There are three main types of skin cancer:
Basal Cell Carcinoma (BCC): This is the most common form of skin cancer, typically appearing as a small, shiny bump or sore that doesn't heal. It grows slowly and rarely spreads to other parts of the body.
Squamous Cell Carcinoma (SCC): This type often appears as a firm, red nodule or a flat sore with a scaly crust. SCC can be more aggressive than BCC and may spread if not treated.
Melanoma: The most dangerous form of skin cancer, melanoma develops from melanocytes, the cells that produce pigment. It can appear as a new mole or change in an existing mole and can spread to other parts of the body if not caught early.
Risk Factors for Skin Cancer
Several factors can increase the risk of developing skin cancer:
UV Exposure: Prolonged exposure to the sun or artificial UV sources increases the risk.
Skin Type: Individuals with fair skin, light hair, and light eyes are at higher risk.
Family History: A family history of skin cancer can increase one’s risk.
Age: The risk of skin cancer increases with age, although it can occur in younger individuals.
Weakened Immune System: Those with weakened immune systems, such as organ transplant recipients, are at greater risk.
The Importance of Self-Skin Exams
Regular self-skin exams are crucial for early detection of skin cancer. Here are some key points regarding their importance:
Early Detection: Identifying changes in your skin early can lead to more effective treatment.
Awareness: Familiarizing yourself with your skin can help you notice new moles or changes in existing ones.
Empowerment: Taking charge of your skin health encourages proactive behaviors and awareness of risk factors.
Annual Skin Checks
In addition to self-exams, annual skin checks by a dermatologist are essential for comprehensive skin health monitoring. The benefits include:
Professional Evaluation: A Dermatology NP can identify suspicious lesions that may not be visible to the untrained eye.
Personalized Advice: A dermatology NP can provide tailored recommendations based on your skin type and risk factors.
Peace of Mind: Regular check-ups can reduce anxiety about skin cancer and provide reassurance about skin health.
Conclusion
Being proactive about skin health through self-exams and regular dermatology visits is critical in reducing the risk of skin cancer. Awareness of risk factors and early detection can save lives, making it essential to prioritize skin checks as part of your health routine.

Skin Tags
Skin Tags
Skin tags, also known as acrochordons, are small, benign growths that typically appear on the skin's surface. They are usually flesh-colored or slightly darker and can vary in size. Skin tags are most commonly found in areas where skin rubs against skin or clothing, such as the neck, armpits, eyelids, and groin.
Causes of Skin Tags
Friction: Areas of skin rubbing against each other can lead to the development of skin tags.
Genetics: A family history of skin tags may increase the likelihood of developing them.
Hormonal changes: Hormonal fluctuations, particularly during pregnancy, can contribute to the formation of skin tags.
Obesity: Overweight individuals are more prone to developing skin tags due to increased friction in skin folds.
Treatment Options
Freezing: Cryotherapy involves freezing the skin tag with liquid nitrogen.
Cutting: A healthcare professional can excise the skin tag using sterile instruments.
Electrosurgery: This method uses electrical currents to remove the skin tag.
Home remedies: Some people use over-the-counter solutions or natural remedies, although these may not be as effective.
Picture Source: DermNet. (2026). https://dermnetnz.org/topics/skin-tag-images

Warts
Warts: Overview
Warts are small, benign (non-cancerous) growths on the skin caused by the human papillomavirus (HPV). They can appear in various forms, including:
Common warts: Rough, raised bumps typically found on fingers, elbows, or knees.
Plantar warts: Hard, grainy growths on the soles of the feet, often causing discomfort.
Flat warts: Small, smooth, flat-topped bumps that can appear in large numbers, usually on the face, neck, or legs.
Filiform warts: Long, narrow growths that usually appear on the face or neck.
Genital warts: Soft, fleshy growths that occur in the genital and anal areas.
What Causes Them
Warts are caused by an infection with HPV, which is highly contagious. The virus can enter the skin through small cuts or abrasions. Factors that can increase the risk of developing warts include:
Weakened immune system
Direct contact with warts (either self-transmission or from others)
Walking barefoot in communal areas (e.g., swimming pools, gyms)
Skin-to-skin contact with someone who has warts
Possible Treatments
While many warts may resolve on their own without treatment, various options are available for those seeking removal:
Over-the-counter treatments: Salicylic acid preparations can help peel away the wart over time.
Cryotherapy: Freezing the wart with liquid nitrogen, causing it to fall off.
Electrosurgery: Burning the wart with electrical currents.
Laser therapy: Using lasers to destroy wart tissue.
Prescription medications: Topical treatments such as imiquimod may be prescribed to stimulate the immune system.
Patient Education
For patients dealing with warts, education is essential for prevention and management:
Practice good hygiene, including regular handwashing.
Avoid sharing personal items like towels, razors, or shoes.
Keep feet dry and use antifungal powders if prone to foot warts.
Consider wearing shoes in communal areas to reduce exposure.
If warts are painful, persistent, or spreading, consult a healthcare professional for evaluation and treatment options.
Picture Source: DermNet (2026). https://dermnetnz.org/topics/viral-warts-images

Wrinkles
What Causes Wrinkles?
Wrinkles are a natural part of aging, but several factors can contribute to their formation:
Age: As skin ages, it loses collagen and elastin, which are essential for maintaining skin's firmness and elasticity.
Sun Exposure: Ultraviolet (UV) rays from the sun can damage skin and accelerate the aging process.
Smoking: Tobacco smoke contains toxins that can damage collagen and elastin, leading to premature wrinkles.
Repetitive Facial Expressions: Frequent movements, such as squinting or frowning, can lead to fine lines over time.
Dehydration: Lack of moisture can make skin appear more wrinkled.
Genetics: Family history can play a role in how and when wrinkles develop.
Environmental Factors: Pollution and other environmental stressors can contribute to skin aging.
Cosmetic Treatment Options
There are various cosmetic treatments available to reduce the appearance of wrinkles:
Botox: Injections of botulinum toxin can temporarily paralyze muscles, reducing the appearance of fine lines.
Dermal Fillers: Substances like hyaluronic acid can be injected to plump up the skin and fill in wrinkles.
Chemical Peels: These treatments involve applying a chemical solution to exfoliate the skin, revealing smoother skin underneath.
Laser Resurfacing: Laser treatments can stimulate collagen production and improve skin texture.
Microdermabrasion: A non-invasive procedure that exfoliates the skin, improving its appearance.
Facelifts: Surgical options that can provide more dramatic and long-lasting results.
Skin Care Recommendations
In addition to cosmetic treatments, a good skincare routine can help prevent and reduce wrinkles:
Moisturize Regularly: Use a hydrating moisturizer to keep skin plump and reduce the appearance of fine lines.
Use Sunscreen: Apply a broad-spectrum sunscreen daily to protect skin from UV damage.
Incorporate Antioxidants: Products containing vitamins C and E can help fight free radicals and improve skin health.
Retinoids: Over-the-counter or prescription retinoids can promote cell turnover and collagen production.
Stay Hydrated: Drink plenty of water to maintain skin hydration from the inside out.
Healthy Diet: A balanced diet rich in fruits, vegetables, and healthy fats can support skin health.
Avoid Smoking: Quitting smoking can significantly improve skin appearance and health.




